Have you ever listened to the song "Have a Drink on Me" by ACDC? I'm just joshing, of course you have! If not, then maybe I'm talking to the wrong generation... However, there is something nostalgic about classic rock songs that bring me back to the fond memories of good times with good people: lake trips, beach bonfires, backyard barbeques and even the occasional wedding reception (although in my opinion, "Mony Mony" by Billy Idol is the all time classic wedding hit). Still, no matter the situation, alcohol seems to be the recurrent factor involved in many of these celebrations. This is for good reason too, as one could argue that it is the quintessential social stimulant that helps bring people together at gatherings. From the elegantly decanted vino, to the aromatically balanced brew or the even the simple yet smooth old-fashioned whiskey; everyone has a unique preference on their choice of drink. So what category do you belong to?
 | ||
| Part of the 53%! I'd like to think of myself a beer connoisseur. (C) World Health Organization 2011. |
Any way you shake it (James Bond pun definitely intended), alcohol is infused into the human dynamic and has been since the dawn of civilization. It should be of no surprise then, as to the curiosity that accompanies attempting to unravel the underlying physiological mechanisms that proliferate our feelings of euphoria upon drinking this magical elixir. Therefore, my aim here is to i) briefly attempt to define what alcohol consumption is and the economic relevance behind our obsession with it, in order to ii) provide a context for the absorption, metabolism and the effector targets as alcohol is consumed and is transported throughout the body (by this I simply mean the organs involved in the "booze cruise," of alcohol through the body). Aboard this luxury booze cruise, we'll be making some pit stops at several tissues along the ethanol route, to see how alcohol affects the system(s) involved: a) the blood, and the b) liver. To make it interesting, I've decided to break up these two sections into three parts:
- The Good- interesting factoid about the physiology of drinking that you could tell your friends about next time your putting a few back.
- The Bad- Obvious as it sounds, I'll include some information that coincides with the consequences of drinking.
- The Atrofreaking kidding me? This final section I'll introduce some recent research developments that may or may not shock you about the consumption of alcohol.
Obviously, the field of alcohol research is very complex and if you're bummed about me skipping the brain, then feel free to check out this simple tutorial about how alcohol effects the brain (narrated by a dude with an Aussie accent to make it sound sweet):
Alcohol effects on the brain
I) What is alcohol consumption and why should I care?
It may cost you if you don't: according to the U.S. Public Health Service Guidelines, the economic cost of drinking in the USA in 2006:- $223.5 billion
- This statistic includes the cost of healthcare, legal and government fees in addition to the actual consumption of alcohol.
- 0.6 fl oz (18 mL) or 14 g of pure alcohol
 |
| Another way to look at it. Image taken from NIAAA: www.niaaa.nih.gov |
- Light drinking = 0-33 (g) EtOH/day
- ~2.5 beers
- Moderate drinking = 34-49 (g) EtOH/day
- ~ 3.5 beers
- Heavy drinking = > 50 (g) EtOH/day
- > 4 beers
Question: How does this relate to the Blood Alcohol Concentration (BAC)?
The BAC is a relationship based on the concentration of alcohol within the blood. Since alcohol is readily absorbed in the bloodstream it is determined by the percentage of alcohol (g) / volume of blood (mL). Everyone has an image of drunk driving tests when they think of BAC:
 |
| He's thinking: "Man, if only I remembered the Widmark equation..." (Image taken from www.fieldsobrietytests.org) |
BAC = ((0.806 x SD)/(BW x Wt)) -(MR x DP)
- 0.806 = Mean water weight in the body
- SD = Number of standard drinks (g)
- BW = Body water constant (Male = 0.58; Female = 0.49)
- Wt = Weight in kg
- MR = Depends on drinking habits (example: average moderate male = 0.017)
- DP = Time of drinking (in hours)
For example: I'm a 135 lb male (61 kg). Let's say I put down three beers over 2 hours. My theoretical BAC then should be:
- 0.009% (or 0.009 g/mL)
Pretty Cool Huh!
II) Booze Cruise: The Good, the Bad, and the Atrofreaking kidding me?
 |
| Taken from www.healthcentral.com. |
- the concentration of alcohol that enters the small intestine.
- Blood flow/heart rate
- Food in the stomach*
*Everyone's heard of eating before you drink to not get too drunk and here's why:
- There is absorption of alcohol within the entire gastrointestinal tract (meaning all the way from your mouth to the rectum), but primarily depends on the retention of alcohol in the stomach, which is effected by the amount of food present. This is because the small intestine represents the area of greatest absorption of alcohol!
- Effect on Antidiuretic hormone (ADH)- Alcohol consumption inhibits your bodies ability to produce a hormone that helps to promote reabsorption of water from the kidneys.
- Effect of increased osmolality- Drinking actually pulls water out of your cells! This is because water flows from a region of low osmolality to high osmolality (meaning that there are more dissolved stuff in your blood than in your cells causing water to move out). Alcohol increases the osmolality of your blood.
a) The Good: Antioxidant can help deter lung-related diseases associated with alcohol consumption:
- Cilia (which are the hairlike projections in your throat that push mucous and other bad stuff out!) show increased damage correlated with alcohol consumption. In a recent study, researchers found that by increasing dietary supplements of two available antioxidants (N-acetylcysteine and procysteine) rats were found to have increased ciliary function in response to alcohol as opposed to rats that just were given alcohol.
- Consumption of alcohol can lead to dilated blood vessels (vasodilation) increasing the rate of blood through the circulatory system. Chronic consumption, however, can have the opposite effect: nitric oxide (NO) is a potent vasodilator and increases in response to small concentrations of alcohol. Increased concentrations of alcohol consumed over time, however, can actually inhibit epithelial cells from producing NO whereby causing increased constriction. It also can activate immune cells to form plaques in the bloodstream leading to heart disease.
- Breast cancer is the leading cause of cancer within women in the United States. Epidemiological data (or the study patterns involved in human health problems) has shown that female heavy drinkers (note the pattern of heavy drinking talked about earlier, which in this case is > 3 standard drinks per day) are equated to a 40-50% increased risk of developing breast cancer. The authors were even quoted to say that around 50,000 cases of breast cancer around the globe has been attributed to increased alcohol consumption!
 |
| RR = relative risk. Taken from Seitz et. al. 2012 |
II) The Liver: The liver is the major site of alcohol metabolism. As the alcohol circulates throughout the bloodstream, it passes through the liver where it is broken down into acetylaldehyde and eventually acetate, which enters the mitochondria for further processing within liver cells
a) The Good: The liver is a powerful organ! Liver cells retain three different mechanisms that can breakdown alcohol, which depend on the amount of alcohol ingested!
Functional components of the liver are called hepatocytes (or liver cells), which facilitate these three different mechanisms:
- Alcohol dehydrogenase (ALDH)- these enzymes are present in the cytosol (the "fluid" inside the cell). At moderate to low concentrations of alcohol, these enzymes breakdown ethanol into acetylaldehyde. This chemical component can then be further broken down into acetate within the mitochondria for energy.
- Microsomal Ethanol-Oxidizing System (EOS)- as the amount of ethanol increases within the blood, ALDH can become "overworked" (or saturated). These microsome EOS systems then are activated (which are present in the smooth endoplasmic reticulum) which breakdown the excess alcohol.
- Peroxisomes- if the levels of alcohol are so high that they become toxic, then the peroxisomes use both ALDH (stored within these vesicles) in addition to hydrogen peroxide to breakdown the excess alcohol.
- Some people develop a alcohol tolerance, after repeated drinking episodes over time. This may be attributed to an up-regulation (increase in synthesis) of ALDH. As more ALDH is present in the cytosol of liver cells, more alcohol can be broken down in the liver. Therefore, as more ALDH is present, the rate at which alcohol in the blood can exert its effects on the brain decreases. This is one reason why some people of the same age, weight or gender can have different tolerances to alcohol.
 |
| Image taken from: www.chemwiki.ucdavis.edu |
Fun Fact (4)- Acetylaldehyde, which is formed during the breakdown of alcohol, can also enter the bloodstream. High concentrations of this substance are also associated with the "hangover effects" in addition to the dehydration and secondary metabolites formed during the breakdown of alcohol.
Fun Fact (5)- Ever wonder why your so hungry after hours of drinking?
- Gluconeogenesis ("Generation of new glucose in the blood) involves multiple enzymatic catalyzed reactions to produce glucose within the liver. The glucose is then released into the blood where brain cells utilize the sugar for energy (your brain solely runs on glucose, with few exceptions). In order for the first set of reactions to take place, however, your liver cells require NADH or the reduced form of the molecule to perform these reactions. If you notice, however, the breakdown of alcohol depletes the NADH reserves in the liver cells and increases the amount of the oxidized form or NAD+. Thus, alcohol causes hypoglycemia (or decrease in glucose levels in the blood) as a direct result of the breakdown of alcohol. So next time you get the munchies after drinking, don't blame your liver cells for getting hungry, since they will be working double time as it is.
b) The Bad: The most common disease associated with alcoholism is the formation of a "fatty liver" (termed hepatic steatosis)-
- During increased consumption of alcohol, the liver undergoes a transformation, in which fat accumulates in the liver (or increases in the amount of triglycerides or "fats"). This may be attributed to the inhibition of fatty acid breakdown (also known as fatty acid oxidation) that occurs within the liver. If an alcoholic continues to drink, they run the risk of fatty liver disease culminating in cirrhosis which is the leading cause of death among heavy drinkers.
 |
| The "white circles" in the fatty liver are fat droplets. Notice that in normal livers, the concentration of these droplets are negligible. |
Fun Fact (6): Use it or gain it? Some people that drink in excess can gain weight. Why is this?
- One reason (among many) that people gain weight during heavy gradual drinking is due to the breakdown of alcohol itself. Earlier, I mentioned that breakdown of alcohol leads to acetylaldehyde which is further processed into acetate in the mitochondria of liver cells. Acetate is a very important molecule as it is a precursor that fuels both TCA cycle (major energy producing pathway) as well as fatty acid anabolic pathway (fatty acid producing pathway). Your cells can "sense" the concentration differences and the energetic demands of the cell: if no energy is required (TCA cycle), then it will be stored as FAT in this case.
- Earlier, I discussed the three mechanisms by which alcohol is broken down in the liver. Chronic consumption of alcohol, however, may lead to the production of reactive oxygen species (ROS). As alcohol is broken down in the liver in high concentrations, the overproduction of acetate (as a result of acetyaldehyde breakdown), in addition to the Microsomal EOS pathway, can lead to the production of ROS. These ROS may also activate inflammatory cascades leading to the activation of cells involved in the production of cytokines (white blood cell signals). These cytokines, in turn, then activate immune cells called Kupffer cells. These cells normally respond to gram negative bacteria and express a protein called Tumor necrosis factor alpha. Normally, this protein would be produced to help preclude the threat of infection by killing infected cells. However, overproduction of this component could lead to the breakdown of liver tissue (called hepatic necrosis) which is thought to contribute to alcoholic liver disease (ALD).
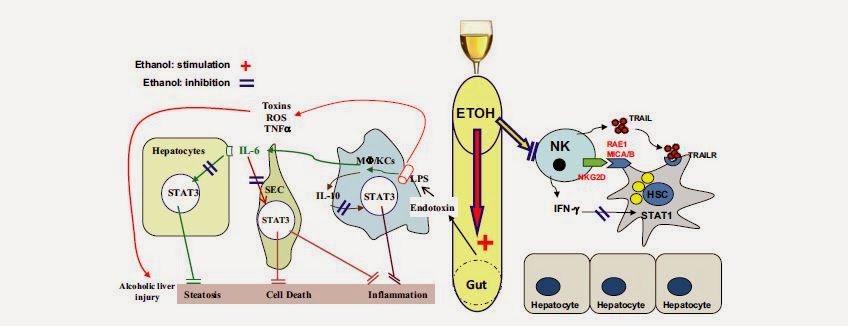 | |
| Taken from Miller et. al. 2011. Overexpression of Tumor Necrosis Factor as a result of alcohol can kill liver cells. |
Alcoholism will continue to be a hotly debated topic, as long as our demand for the substance continues. However, this is not to say that drinking is all that bad. In fact, there are some benefits to drinking: I) earlier I mentioned that antioxidants can lead to decreased damage to cilia within the throat. Wine actually contains a high amount of antioxidants. II) In addition, wine contains a substance called resveratrol which has been shown to activate proteins involved in the breakdown of reactive oxygen species (the very thing activated in liver cells as a result of increased alcohol consumption...Go figure right?). It really all depends on moderation. Please note, however, this is not meant to completely deter you from enjoying your favorite alcoholic beverage (in fact, as soon as I'm finished writing this, I'll probably enjoy a cold one myself!). I mainly wanted to illustrate some of the issues that can be attributed to the consumption of alcohol, as well as to spur interest into the mechanisms that occur within our bodies as a result. So next time your about to "have yourself a brew," (-to quote the immortal Johny Cash), have a drink on me...But perhaps, just make it one ;).
Citations
Ambade, A and P. Mandrekar. 2011. Oxidative stress and inflammation: essential partners in alcoholic liver disease. International Journal of Hepatology. Article ID: 853175, 9 pages.
Barclay, G. A, J. Barbour, S. Stewart. C. P. Day and E. Gilvarry. 2008. Adverse physical effects of alcohol misuse. Advances in Psychiatric Treatment 14: 139-151.
Bouchery, E. E, M. S. Henrik, J. Harwood, J. J. Sacks, C. J. Simon and R. D. Brewer. 2011. Economic costs of excessive alcohol consumption in the U.S., 2006. American Journal of Preventative Medicine 41 (5): 516-524.
Cahill, P. A and E. M. Redmond. 2012. Alcohol and cardiovascular disease: modulation of vascular cell function. Nutrients 4: 297-318.
Crow, K.E and R. D. Batt. Human metabolism of alcohol. Volumes I-III. Boca Raton, FL. CRC Press. 1989.
Eckardt, M. J, S. E. File, G. L. Gessa, K. A. Grant, C. Guerri, P. L. Hoffman, H. Kalant, G. F. Koob, T-K. Li and B. Tabakoff. 1998. Effects of moderate alcohol consumption on the central nervous system. Alcoholism: Clinical and Experimental Research 22 (5): 998-1040.
Gastineau, C. F, W. J. Darby and T. B. Turner. Fermented food beverages in nutrition. New York, NY. Academic Press. 1979.
Kypri, K, J. Langley and S. Stephenson. 2005. Episode centered analysis of drinking to intoxication in university students. Alcohol & Alcoholism 40 (5): 447-452.
Lieber, C. S. Medical and nutritional complications of alcoholism: mechanisms and management. New York, NY. Plenum Medical Book Company. 1992.
Miller, A.M, N. Horiguchi, W-I. Jeong, S. Radaeva and B. Gao. 2011. Molecular mechanisms of alcoholic liver disease: innate immunity and cytokines. Alcoholism: Clinical and Experimental Research 35 (5): 787-793
Seitz, H. K, C. Pelucchi, V. Bagnardi and C. L. Vecchia. 2012. Epidemiology and pathophysiology of alcohol and breast cancer. Alcohol & Alcoholism 47 (3): 204-212.
Simet, S. M., J. A. Pavlik and J. H. Sisson. 2013. Dietary antioxidants prevent alcohol-induced ciliary dysfuntion. Alcohol 47: 629-635.
I was searching all over the internet to get natural remedies for hangovers, I tried a number of them never really being impressed by the result. I tried a sample of Detoxicated at a holiday party and actually noticed a difference in my recovery the next day.
ReplyDelete